2. 上海市嘉定区妇幼保健院妇女保健科 上海 201812;
3. 上海市嘉定区妇幼保健院检验科 上海 201812;
4. 上海市普陀区疾病预防控制中心 上海 200333
2. Department of Women Health Care, Maternal and Child Health Care Hospital of Jiading District, Shanghai 201812, China;
3. Department of Clinical Laboratory, Maternal and Child Health Care Hospital of Jiading District, Shanghai 201812, China;
4. Putuo Center for Disease Control and Prevention, Shanghai 200333, China
随着城市化带来环境污染的加剧,有毒重金属镉(cadmium, Cd)通过生殖毒性作用对母婴健康的危害日益受到关注。人体主要通过食用镉污染食物,主动或被动吸入烟草烟雾,以及有色金属工业的职业暴露而接触镉[1]。膳食中钙、铁、锌等微量营养素匮乏的人受到的镉毒性作用可能更明显[2]。胎盘虽是良好屏障,但镉仍有可能在胎儿体内积聚[3],并干扰胎盘转运必需营养素而影响胎儿生长发育[4]。既往研究很少在孕前检测妇女血镉浓度,并于孕期和产时重复测量,以阐述血镉水平的动态变化趋势。本研究以上海市嘉定区妇女及新生儿为研究对象,检测妇女从孕前至孕期的全血和脐血镉浓度,分析孕期血镉和脐血镉水平的影响因素,为促进妇幼健康提供科学依据。
资料和方法研究对象 本研究以复旦孕前队列研究(PLOTS)为基础,自2016年于上海市嘉定区妇幼保健院招募了逾1000对孕前夫妇,纳入标准:(1)参加孕前检查;(2)计划怀孕;(3)至少一方为当地常住居民。队列通过基线招募和随访收集夫妇孕前、孕期和分娩生物样本,自编问卷收集夫妇孕前和孕晚期社会人口、体格测量和生活方式等信息。本研究共纳入2016年9月至2018年3月参加队列并分娩单胎活产儿的92名妇女,对92组从孕前、孕中期至孕晚期的全血和分娩脐血共计368份血样的镉浓度进行检测。本研究获得复旦大学公共卫生学院伦理委员会批准,所有研究对象均签署知情同意书。
在妇女孕前(距末次月经平均10周)、孕中期(距末次月经平均20孕周)和孕晚期(距末次月经平均32孕周)各采集3 mL静脉血,分娩时(距末次月经平均40孕周)留取3 mL脐静脉血,采用EDTA-K2抗凝,颠倒混匀后于-80 ℃保存。
检测方法 血样中8种元素,包括镉(Cd)、铅(Pb)、钙(Ca)、铁(Fe)、锌(Zn)、铜(Cu)、锰(Mn)、硒(Se)的浓度均采用Agilent 7700X电感耦合等离子体质谱仪(美国Agilent公司)测定。取室温复融血样100 μL,加入1.90 mL含0.01%(V/V)Triton X-100(德国Merck公司)和0.01%(V/V)HNO3(MOS级,德国Merck公司)的稀释剂。Multi Reax漩涡振荡器(德国Heidolph公司) 1 000 rpm涡旋振荡5 min; Microfuge 16离心机(美国Beckman Coulter公司), 16 160×g离心5 min,取上清液上机检测。通过标准曲线法定量测定,每个样本重复测量3次,同时设试剂空白对照。在线加入含铟(In)、钪(Sc)和锗(Ge)的混合内标以校正基线干扰和漂移。
统计学分析 通过EpiData 3.1进行数据双录入,用SAS 9.4软件进行分析。用M(P25~P75)描述不符合正态分布的数据,用x±s描述符合正态分布的数据,构成比以n(%)描述。以Friedman检验进行4次重复测量多组间血镉浓度差异的比较,以q检验进行两两比较。通过协方差矩阵为无结构相关的混合线性模型,以最小方差二次无偏倚估计法估计参数,筛选孕期血镉和脐血镉水平的影响因素,以最小二乘均值差分两两比较各时点间血镉浓度的差异。P < 0.05为差异有统计学意义。
结果一般情况 92名妇女孕前平均年龄28.00(25.50~29.00)岁,孕前平均体重指数(body mass index, BMI)20.30(19.10~22.25)kg/m2,孕期平均增重(14.83±4.30)kg,孕期均无主动吸烟和饮酒(表 1)。
| Characteristics | Case [n (%)] |
| Age before pregnancy (y) | |
| ≥30 | 20 (21.74) |
| < 30 | 72 (78.26) |
| Household registration | |
| Shanghai | 56 (60.87) |
| Non-Shanghai | 36 (39.13) |
| Education level | |
| Bachelor’s degree or above | 63 (68.48) |
| Below bachelor’s degree | 29 (31.52) |
| Family income per capita (yuan/y) | |
| ≥100 000 | 55 (59.78) |
| < 100 000 | 37 (40.22) |
| Pre-pregnancy BMI (kg/m2) | |
| Underweight (< 18.5) | 14 (15.22) |
| Normal weight (18.5-) | 67 (72.83) |
| Overweight or obese (≥24.0) | 11 (11.96) |
| Passive smoking before pregnancy | |
| Yes | 27 (29.35) |
| No | 65 (70.65) |
| Passive smoking during pregnancy | |
| Yes | 6 (6.52) |
| No | 86 (93.48) |
| Gestational weight gain | |
| Inadequate | 17 (18.48) |
| Appropriate | 41 (44.57) |
| Excessive | 34 (36.96) |
| Supplementation of Ca/Fe/Zn during pregnancy | |
| Yes | 73 (79.35) |
| No | 19 (20.65) |
| Supplementation of vitamin during pregnancy | |
| Yes | 71 (77.17) |
| No | 21 (22.83) |
| Drinking juice during pregnancy | |
| At least once per week | 16 (17.39) |
| Less than once per week | 76 (82.61) |
| Drinking milk or eating cheese during pregnancy | |
| At least 4 times per week | 52 (56.52) |
| Less than 4 times per week | 40 (43.48) |
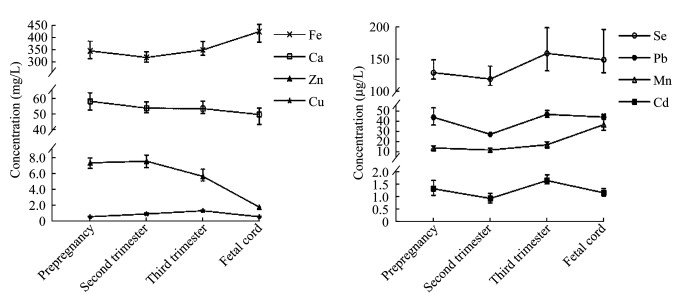
妇女孕前至孕晚期血镉和脐血镉浓度 除脐血钙、孕中期母血锌和血铜浓度呈正态分布外,其余元素浓度均呈非正态分布,故以M(P25~P75)描述元素浓度的分布(表 2和图 1)。Friedman检验结果显示,血镉浓度在4个时点间的差异有统计学意义(M=152.30,P < 0.01)。q检验结果显示,孕中期血镉浓度低于孕前(q=15.03,P < 0.01),孕晚期血镉浓度高于孕中期(q=25.27,P < 0.01),脐血镉浓度低于孕晚期(q=15.75,P < 0.01)。所有血样镉浓度均未超过WHO推荐的一般人群参考值5 μg/L[5]。
| (μg/L) | |||||||||||||||||||||||||||||
| Group | Case (n) | Median | P25-P75 | Range | |||||||||||||||||||||||||
| Preconception | 92 | 1.32 | 1.07-1.63 | 0.72-2.78 | |||||||||||||||||||||||||
| Second trimester | 92 | 0.94 | 0.76-1.13 | 0.31-2.25 | |||||||||||||||||||||||||
| Third trimester | 92 | 1.65 | 1.51-1.87 | 1.07-3.38 | |||||||||||||||||||||||||
| Fetal cord | 92 | 1.16 | 1.04-1.34 | 0.80-2.66 | |||||||||||||||||||||||||
|
| The concentrations of elements were shown as Media (P25-P75). 图 1 妇女孕前至孕晚期全血及新生儿脐血元素浓度变化趋势 Fig 1 The element pattern in women's blood from preconception to the third trimester and fetal cord blood |
孕期血镉和脐血镉浓度的影响因素 混合线性模型结果显示孕前血镉水平与孕期血镉和脐血镉水平呈正相关(P < 0.01)。与孕中期相比,孕晚期血镉浓度增加(P < 0.01);与孕晚期相比,脐血镉浓度降低(P < 0.01);与孕中期相比,脐血镉浓度增加(P < 0.01)。孕期至分娩的血镉与血锰水平呈负相关(P < 0.01)。上海本地户籍、大学及以上文化程度和孕期喝纯果蔬汁至少每周1次的妇女孕期血镉和脐血镉浓度较低(P < 0.05),孕期被动吸烟的妇女孕期血镉和脐血镉浓度较高(P<0.05), 其余变量如孕前年龄、家庭人均年收入、孕前被动吸烟、孕前BMI、孕期增重、孕期补充维生素、孕期补充钙/铁/锌和孕期喝奶或吃奶酪与孕期血镉和脐血镉浓度均无显著关联(表 3~4)。
| Variables | β | 95%CI | SE | t | P |
| Time point | |||||
| Second trimester | Ref | - | - | - | - |
| Third trimester | 0.786 | 0.706-0.865 | 0.040 | 19.62 | < 0.001 |
| Cord | 0.452 | 0.305-0.599 | 0.074 | 6.11 | < 0.001 |
| Concentration of Cd before pregnancy | 0.257 | 0.145-0.368 | 0.056 | 4.57 | < 0.001 |
| Concentrations of Mn in maternal blood and cord blood | -0.007 | -0.011-(-0.002) | 0.002 | -3.13 | 0.003 |
| Household registration | |||||
| Shanghai | -0.112 | -0.204-(-0.020) | 0.046 | -2.41 | 0.018 |
| Non-Shanghai | Ref | - | - | - | - |
| Drinking juice during pregnancy | |||||
| At least once per week | -0.129 | -0.244-(-0.015) | 0.057 | -2.25 | 0.028 |
| Less than once per week | Ref | - | - | - | - |
| Education level | |||||
| Bachelor’s degree or above | -0.108 | -0.214-(-0.002) | 0.053 | -2.03 | 0.046 |
| Below bachelor’s degree | Ref | - | - | - | - |
| Passive smoking during pregnancy | |||||
| Yes | 0.182 | 0.003-0.362 | 0.090 | 2.02 | 0.047 |
| No | Ref | - | - | - | - |
| Passive smoking before pregnancy | |||||
| Yes | -0.083 | -0.188-0.023 | 0.053 | -1.56 | 0.122 |
| No | Ref | - | - | - | - |
| Gestational weight gain | |||||
| Inadequate | -0.104 | -0.235-0.027 | 0.066 | -1.58 | 0.119 |
| Appropriate | Ref | - | - | - | - |
| Excessive | 0.021 | -0.085-0.126 | 0.053 | 0.39 | 0.697 |
| Pre-pregnancy BMI (kg/m2) | |||||
| Underweight (< 18.5) | 0.0003 | -0.1295-0.1302 | 0.065 | 0.01 | 0.996 |
| Normal weight (18.5-) | Ref | - | - | - | - |
| Overweight or obese (≥24.0) | -0.060 | -0.200-0.081 | 0.070 | -0.85 | 0.400 |
| Supplementation of vitamin during pregnancy | |||||
| Yes | 0.060 | -0.060-0.180 | 0.060 | 0.99 | 0.326 |
| No | Ref | - | - | - | - |
| Supplementation of Ca/Fe/Zn during pregnancy | |||||
| Yes | -0.021 | -0.136-0.095 | 0.058 | -0.35 | 0.725 |
| No | Ref | - | - | - | - |
| Drinking milk or eating cheese during pregnancy | |||||
| At least 4 times per week | -0.042 | -0.136-0.051 | 0.047 | -0.90 | 0.369 |
| Less than 4 times per week | Ref | - | - | - | - |
| Age before pregnancy (y) | |||||
| ≥30 | 0.039 | -0.076-0.154 | 0.058 | 0.68 | 0.501 |
| < 30 | Ref | - | - | - | |
| Family income per capita (yuan/y) | |||||
| ≥100 000 | 0.014 | -0.094-0.121 | 0.054 | 0.25 | 0.802 |
| < 100 000 | Ref | - | - | - | - |
| Pairwise comparison group | β | 95%CI | SE | t | P |
| Third trimester vs. Second trimester | 0.786 | 0.706-0.865 | 0.040 | 19.62 | < 0.001 |
| Cord vs. Second trimester | 0.452 | 0.305-0.599 | 0.074 | 6.11 | < 0.001 |
| Third trimester vs. Cord | 0.334 | 0.195-0.473 | 0.070 | 4.79 | < 0.001 |
本研究中, 上海市嘉定区的92名妇女孕前血镉浓度中位数(1.32 μg/L)高于1998年全国1 139名成年妇女孕前血镉浓度中位数(0.83 μg/L)[6],略低于2009—2010年南京市120名非孕妇女孕前血镉浓度平均数(1.65 μg/L)[7];孕中期血镉浓度中位数(0.94 μg/L)低于2009—2010年南京市174名孕妇孕中期血镉浓度平均数(1.63 μg/L)[7];孕晚期血镉浓度中位数(1.65 μg/L)和脐血镉浓度中位数(1.16 μg/L)略高于2006—2007年上海市和大连市241对母婴孕晚期血镉浓度中位数(1.1 μg/L)和脐血镉浓度中位数(0.6 μg/L)[8]及2011年上海市400对母婴孕晚期血镉浓度平均数(1.15 μg/L)和脐血镉浓度平均数(0.82 μg/L)[9]。目前上海市嘉定区妇女孕前至孕期血镉及胎儿脐血镉水平总体较低,但较过去十年可能有所上升。
孕中期血镉浓度较孕前降低(P < 0.01),孕中期至孕晚期血镉水平呈现上升趋势(P < 0.01),脐血镉浓度低于母血镉浓度(P < 0.01)。一项417对孕妇和非孕妇匹配的研究发现孕期前半程的血镉浓度显著低于孕前血镉浓度[10],可能与孕期血浆容量扩大等原因导致血液元素浓度生理性稀释有关。非洲国家贝宁南部地区32名孕妇的研究结果显示分娩时血镉浓度显著高于孕早期血镉浓度(P < 0.01),可能与孕妇体内铁水平下降导致二价金属离子转运蛋白1上调和镉转运增加有关[11]。也有研究发现孕期血镉水平无显著差异[7]。胎盘具有对镉的屏障作用,胎盘中的金属硫蛋白能与镉结合并减少其向胎儿的转移,使脐血镉比母血镉低[12]。鉴于孕母全血镉浓度和胎儿脐血镉浓度在孕期的变化特征,单次测量不足以描述整个孕期的镉水平,提示未来相关研究应考虑血样采集时点的因素。
孕前血镉水平与孕期血镉和脐血镉水平呈正相关(P < 0.01),可能由于镉在人体内的半衰期长达10~30年且排出缓慢[13]。孕期至分娩血镉浓度与血锰浓度呈负相关(P < 0.01),而国外研究发现血镉和血锰水平间的关系为倒U形[14]。上海本地户籍的妇女孕期血镉和脐血镉水平较低(P < 0.05),可能与上海是镉非污染区[15]、嘉定区饮用水源地水中镉浓度达标[16]和土壤未受重金属污染[17]等有关。孕期每周至少喝一次纯果蔬汁的妇女孕期血镉和脐血镉水平较低(P < 0.05),动物实验也发现葡萄汁或苹果汁对镉染毒大鼠具有保护作用[18]。大学及以上文化程度的妇女孕期血镉和脐血镉浓度较低(P < 0.05),孕期被动吸烟的妇女血镉和脐血镉浓度较高(P < 0.05),与朱泓等[9]的研究结论一致。文化水平较高的妇女可能更了解重金属的危害且拥有较好的居住和工作环境,因此镉暴露较少。2012年来自中国7个城市的1 145份问卷调查显示,烟草平均镉含量为3.06 μg/g[19],孕期被动吸烟会使脐血镉水平明显升高[20]。年龄、补锌、孕期喝牛奶、饮用自来水、使用化妆品和新生儿性别等因素可影响孕期血镉和脐血镉水平[9, 21]。
本研究通过测量妇女从孕前至孕期全血和脐血镉浓度,描述孕前、孕期血镉和脐血镉水平的变化趋势和影响因素。上海市嘉定区妇女孕前至孕期血镉及脐血镉总体处于较低水平。孕期血镉水平呈先降后升的变化趋势,脐血镉水平低于孕晚期血镉水平。围孕产期应重视合理营养,减少烟草镉暴露,并加强镉监测以促进母婴健康。本研究的样本量较小,将来需要更大样本量的研究进一步探索围孕期、孕期和脐血的血镉水平及影响因素。
| [1] |
WORLD HEALTH ORGANIZATION.International programme on chemical safety-cadmium[EB/OL].[2018-10-17].http://www.who.int/ipcs/assessment/public_health/cadmium/en/.
|
| [2] |
PERAZA MA, AYALA-FIERRO F, BARBER DS, et al. Effects of micronutrients on metal toxicity[J]. Environ Health Perspect, 1998, 106(Suppl 1): 203-216.
[URI]
|
| [3] |
GUNDACKER C, HENGSTSCHL GER M. The role of the placenta in fetal exposure to heavy metals[J]. Wien Med Wochenschr, 2012, 162(9-10): 201-206.
[URI]
|
| [4] |
GOYER RA. Toxic and essential metal interactions[J]. Annu Rev Nutr, 1997, 17: 37-50.
[URI]
|
| [5] |
WORLD HEALTH ORGANIZATION.International programme on chemical safety-environmental health criteria 134: cadmium[EB/OL].[2018-10-30].http://www.inchem.org/documents/ehc/ehc/ehc134.htm.
|
| [6] |
郑星泉. 1981-1998年我国女性成人血中铅镉水平变化[J]. 环境与健康杂志, 2001, 18(6): 332-335. [URI]
|
| [7] |
LIU KS, MAO XD, HAO JH. Towards prenatal biomonitoring in Nanjing, China:lead and cadmium levels in the duration of pregnancy[J]. Chin Med J (Engl), 2013, 126(16): 3107-3111.
[URI]
|
| [8] |
施蓉, 王沛, 高宇, 等. 孕妇全血、脐血中微量元素和重金属元素检测及相关性探讨[J]. 上海交通大学学报(医学版), 2010, 30(8): 897-901. [URI]
|
| [9] |
朱泓, 杨祖菁, 曹露露, 等. 妊娠期镉暴露水平对母儿的影响及相关因素分析[J]. 中华临床医师杂志(电子版), 2012, 6(18): 5714-5716. [CNKI]
|
| [10] |
BONITHON-KOPP C, HUEL G, GRASMICK C, et al. Effects of pregnancy on the inter-individual variations in blood levels of lead, cadmium and mercury[J]. Biol Res Pregnancy Perinatol, 1986, 7(1): 37-42.
[URI]
|
| [11] |
GUY M, ACCROMBESSI M, FIEVET N, et al. Toxics (Pb, Cd) and trace elements (Zn, Cu, Mn) in women during pregnancy and at delivery, South Benin, 2014-2015[J]. Environ Res, 2018, 167: 198-206.
[URI]
|
| [12] |
ESPART A, ARTIME S, TORT-NASARRE G, et al. Cadmium exposure during pregnancy and lactation:materno-fetal and newborn repercussions of Cd(ii), and Cd-metallothionein complexes[J]. Metallomics, 2018, 10(10): 1359-1367.
|
| [13] |
刘伟成, 李明云. 镉毒性毒理学研究进展[J]. 广东微量元素科学, 2005, 12(12): 1-5. [URI]
|
| [14] |
OULHOTE Y, MERGLER D, BOUCHARD MF. Sex- and age-differences in blood manganese levels in the U.S.general population:national health and nutrition examination survey 2011-2012[J]. Environ Health, 2014, 13: 87.
[URI]
|
| [15] |
KE S, CHENG X, LI H, et al. Body burden of cadmium and its related factors:a large-scale survey in China[J]. Sci Total Environ, 2015, 511: 649-654.
[URI]
|
| [16] |
陆凤娟. 以嘉定区为例对上海市郊区饮用水源水重金属进行健康风险评价[J]. 中国环境监测, 2013, 29(2): 5-8. [URI]
|
| [17] |
陆凤娟. 上海市郊区两试点村土壤环境质量调查研究[J]. 环境科学与管理, 2015, 40(1): 41-45. [URI]
|
| [18] |
RUIZ PLM, HANDAN BA, de MOURA CFG, et al. Protective effect of grape or apple juices in bone tissue of rats exposed to cadmium:role of RUNX-2 and RANK/L expression[J]. Environ Sci Pollut Res Int, 2018, 25(16): 15785-15792.
[URI]
|
| [19] |
O'CONNOR RJ, SCHNELLER LM, CARUSO RV, et al. Toxic metal and nicotine content of cigarettes sold in China, 2009 and 2012[J]. Tob Control, 2015, 24(Suppl 4): iv55-iv59.
[URI]
|
| [20] |
徐宣枝, 周昌菊, 余丹, 等. 孕期被动吸烟对脐血铅、镉水平的影响[J]. 中国医师杂志, 2006, 8(10): 1333-1335. [URI]
|
| [21] |
古桂雄, 徐培娟, 李丽. 母婴血镉含量及其有关因素的影响[J]. 工业卫生与职业病, 2007, 33(3): 150-153. [URI]
|
 2020, Vol. 47
2020, Vol. 47


