脓毒症(sepsis)是机体对感染的反应失调而导致威胁生命的器官功能障碍[1]。急性肾损伤(acute kidney injury,AKI)被认为是与死亡率独立相关的危重病并发症[2-3]。脓毒症儿童合并AKI发病迅速,死亡率高。目前,AKI诊断标准由2012年KDIGO(Kidney Disease Improving Global Outcomes)发布,通过尿量减少或血肌酐较其基础值升高进行诊断,但掌握肌酐基础值后诊断AKI需要一定时间的观察[4]。应用KDIGO标准诊断AKI仍存在一定数量的漏诊率[5],特别对危重症患者仍存在局限性。除了肌酐和尿量,胱抑素C(cystatin C,CysC)、视黄醇结合蛋白(retinol-binding protein,RBP)也是临床上评价肾功能的常用指标。中性粒细胞明胶酶相关脂质运载蛋白(neutrophil gelatinase-associated lipocalin,NGAL)和肾损伤因子1(kidney injury molecule 1,KIM-1)是近年诊断AKI的新的生物标志物。NGAL最早被报道于先天性心脏病患儿体外循环术后合并AKI时具有早期提示的作用,近年来的研究逐渐关注当其他疾病合并AKI时它是否同样具有良好的诊断价值;KIM-1被认为是一种潜在的AKI标志物,但总体报道少,并多集中在尿液中KIM-1的诊断价值上。两个标志物在危重症儿童AKI中应用的报道均不多。基于AKI是一种与原发疾病息息相关的综合征,同时危重症儿童往往病情复杂,发展迅速,本研究拟通过收集不同时点的样本,对血NGAL和KIM-1指标在脓毒症患儿AKI早期诊断以及特殊治疗过程中的临床应用价值进行探讨。
资料和方法临床资料 连续纳入2019年1—12月诊断脓毒症、入住复旦大学附属儿科医院重症监护室的患儿82例。脓毒症诊断标准按《儿童脓毒性休克(感染性休克)诊治专家共识(2015版)》[6]。按照排(剔)除标准除去13例。排除标准为各类结缔组织病(如类风湿、皮肌炎)、慢性肾脏病(如慢性肾损伤)及肿瘤、免疫缺陷等基础疾病的患儿。剔除标准为住院24 h内死亡或自动出院者。最终纳入脓毒症的患儿69例。根据脓毒症同期是否合并AKI分为脓毒症AKI组和脓毒症非AKI组。AKI的诊断标准按2012年KDIGO发布的48 h内血肌酐升高 > 26.5 μmol/L或大于基础值的1.5倍(确认或推测7天发生)或持续6 h以上尿量少于0.5 mL·kg-1·h-1。根据诊断脓毒症24 h内是否行连续性肾脏替代治疗(continuous renal replacement therapy,CRRT),将脓毒症AKI组进一步分为脓毒症AKI-CRRT组和脓毒症AKI-非CRRT组。CRRT治疗组均采用连续静脉-静脉血液滤过透析模式(continuous venovenous hemodiafiltration,CVVHDF)。超滤量根据临床治疗要求设定在0.5~5 mL·kg-1·h-1,透析量及滤过液量均设定为25 mL·kg-1·h-1 [7-8],将尿量及超滤量相加作为共同的观察指标。本研究获复旦大学附属儿科医院伦理委员会批准(伦理批件号:复儿伦申〔2019〕315)。
研究方法 留取脓毒症AKI和非AKI患儿3个时点(入院后0 h、24 h、72 h)和正常对照组体检时(所用标本为生化检测剩余血清,≤0.5 mL)的静脉血,3 350×g离心5 min,吸取血清放置-70 ℃冰箱保存备用,并检测NGAL、KIM-1、肌酐、CysC、RBP。NGAL和KIM-1检测:采用ELISA方法,试剂为美国R & D公司的Human Lipocalin-2/NGAL Immunoassay和Human Serum TIM-1/KIM-1/HAVCR Immunoassay检测试剂盒。肌酐、CysC、RBP检测:使用美国贝克曼库尔特有限公司AU5800全自动生化仪检测。肌酐检测原理为酶法,CysC和RBP检测原理为免疫浊度法。检测试剂、定标品、质控品均与仪器配套。尿量计量:记录24 h时及之后每个研究观察时点为起点的24 h尿量(mL),以患儿每公斤(kg)每小时(h)的尿量报告(mL·kg-1·h-1);记录脓毒症AKI-CRRT治疗组患儿超滤量(mL),以患儿每公斤(kg)每小时(h)的形式报告(mL·kg-1·h-1),并将两者相加。小样本量方法验证NGAL、KIM-1试剂盒提供的参考区间,纳入正常儿童均为“建立中国儿童临床常规检验指标参考区间”课题招募的正常体检儿童,符合伦理要求[9]。检测纳入研究的22例正常儿童的血NGAL、KIM-1水平,如检测数据有离群值,剔除后补齐验证样本量。检测数据≤2个结果超出待验证区间,验证通过;检测数据 > 3个结果超出待验证区间,则需要检查分析程序,根据参考人群差异自建参考区间[10]。
统计学分析 正态分布的计量资料用x±s表示,非正态分布的计量资料用中位数和四分位间距M(P25,P75)表示。分类资料统计使用χ2检验,组间比较用非参数检验k个独立样本Kruskal-Wallis H比较,脓毒症AKI-CRRT组各时点间的比较用Friedman非参数检验。使用受试者工作特征(ROC)曲线评价肌酐、尿量、NGAL、KIM-1、CysC和RBP对AKI患儿的诊断价值,取约登指数最大时的灵敏度和特异性。以双侧检验P < 0.05为差异有统计学意义。所有数据均使用SPSS 22.0软件分析,Graphad Prism8软件绘制箱式图。
结果临床资料 脓毒症AKI组28例,住院天数9~175天(M=23天)。脓毒症非AKI组41例,住院天数7~66天(M=25.5天)。脓毒症AKI组中进行CRRT治疗者18例,脓毒症AKI与非AKI患儿的临床信息见表 1。正常对照组:选取同期体检的健康儿童共22例(男性12例,女性10例),其中 < 1岁9例,1~4岁4例,5~9岁3例,≥10岁6例。正常对照组年龄和性别与病例组差异无统计学意义。
| [n(%)] | |||||||||||||||||||||||||||||
| Characteristics | Sepsis AKI group(n=28) | Sepsis non-AKI group(n=41) | χ2 | P | |||||||||||||||||||||||||
| Age | 2.818 | 0.421 | |||||||||||||||||||||||||||
| < 1 y | 9 (32.1) | 8 (19.5) | |||||||||||||||||||||||||||
| 1-4 y | 8 (28.6) | 15 (36.6) | |||||||||||||||||||||||||||
| 5-9 y | 9 (32.1) | 11 (26.8) | |||||||||||||||||||||||||||
| ≥10 y | 2 (7.1) | 7 (17.1) | |||||||||||||||||||||||||||
| Gender | 0.348 | 0.365 | |||||||||||||||||||||||||||
| Female | 15 (53.6) | 19 (46.3) | |||||||||||||||||||||||||||
| Male | 13 (46.4) | 22 (53.7) | |||||||||||||||||||||||||||
血NGAL、KIM-1参考区间验证 NGAL试剂盒参考区间42~177 ng/mL,检测数据41.18~57.98 ng/mL,均值(49.5±4.44)ng/mL,1例超出待验证区间,验证通过。KIM-1试剂盒参考区间0~56.9 pg/mL,检测数据14.04~52.39 pg/mL,均值(31.43±9.86)pg/mL,均未超出待验证区间,验证通过。采用验证通过的区间作为本研究的正常参考区间。
脓毒症AKI患儿各指标的检测结果 NGAL在脓毒症AKI组和脓毒症非AKI组各时点的检测水平均高于正常对照组,脓毒症AKI组显著高于脓毒症非AKI组(P均 < 0.05)。24 h、72 h时脓毒症AKI和非AKI患儿的KIM-1均高于正常对照组,这2个时点脓毒症AKI患儿的KIM-1显著高于脓毒症非AKI患儿(P均 < 0.05)。肌酐在3个时点、CysC和RBP在后2个时点时,脓毒症AKI组均明显高于非AKI组(P均 < 0.05,表 2)。
| [M (P25, P75)] | |||||||||||||||||||||||||||||
| Index | Sepsis AKI | Sepsis non-AKI | Normal control group | P1 | P2 | P3 | |||||||||||||||||||||||
| NGAL (ng/mL) | |||||||||||||||||||||||||||||
| 0 h | 111.34 (102.36, 133.27) | 82.42 (66.59, 96.35) | 49.70 (46.85, 52.38) | < 0.001 | < 0.001 | < 0.001 | |||||||||||||||||||||||
| 24 h | 167.20 (142.61, 190.22) | 91.10 (74.09, 108.40) | < 0.001 | < 0.001 | < 0.001 | ||||||||||||||||||||||||
| 72 h | 169.47 (136.88, 182.31) | 91.57 (78.59, 111.34) | < 0.001 | < 0.001 | < 0.001 | ||||||||||||||||||||||||
| KIM-1 (pg/mL) | |||||||||||||||||||||||||||||
| 0 h | 114.63 (94.04, 245.63) | 89.96 (68.87, 111.31) | 29.74 (26.67, 34.99) | < 0.001 | < 0.001 | 0.178 | |||||||||||||||||||||||
| 24 h | 223.23 (127.42, 330.72) | 89.21 (71.22, 119.19) | < 0.001 | < 0.001 | 0.001 | ||||||||||||||||||||||||
| 72 h | 400.26 (210.62, 486.55) | 91.25 (68.76, 126.05) | < 0.001 | < 0.001 | < 0.001 | ||||||||||||||||||||||||
| Creatinine (μmol/L) | |||||||||||||||||||||||||||||
| 0 h | 57.00 (42.00, 72.00) | 35.00 (27.00, 42.00) | 29.00 (23.00, 54.00) | < 0.001 | 1.000 | < 0.001 | |||||||||||||||||||||||
| 24 h | 100.00 (76.00, 138.00) | 28.0 0(22.00, 35.00) | < 0.001 | 1.000 | < 0.001 | ||||||||||||||||||||||||
| 72 h | 79.00 (51.00, 135.00) | 26.00 (20.00, 33.00) | < 0.001 | 0.354 | < 0.001 | ||||||||||||||||||||||||
| CysC (mg/L) | |||||||||||||||||||||||||||||
| 0 h | 1.10 (0.84, 1.28) | 0.82 (0.65, 1.21) | 0.75 (0.69, 0.93) | 0.035 | 1.000 | 0.087 | |||||||||||||||||||||||
| 24 h | 2.25 (2.04, 2.97) | 0.81 (0.66, 1.21) | < 0.001 | 1.000 | < 0.001 | ||||||||||||||||||||||||
| 72 h | 1.82 (1.15, 2.32) | 0.83 (0.68, 1.10) | < 0.001 | 1.000 | < 0.001 | ||||||||||||||||||||||||
| RBP (mg/L) | |||||||||||||||||||||||||||||
| 0 h | 28.00 (16.30, 32.60) | 21.20 (13.20, 29.50) | 25.1 (22.10, 27.80) | 0.212 | 0.061 | 0.055 | |||||||||||||||||||||||
| 24 h | 32.60 (20.60, 56.00) | 12.10 (10.00, 20.90) | 0.765 | 0.001 | 0.000 | ||||||||||||||||||||||||
| 72 h | 37.60 (22.00, 54.10) | 20.90 (14.50, 25.40) | 0.168 | 0.230 | 0.000 | ||||||||||||||||||||||||
| P1:Sepsis AKI vs. normal control group; P2:Sepsis non-AKI vs. normal control group; P3:Sepsis AKI vs. sepsis non-AKI.NGAL:Neutrophil gelatinase-associated lipocalin; KIM-1:Kidney injury molecule 1;CysC:Cystatin C; RBP:Retinol-binding protein. | |||||||||||||||||||||||||||||
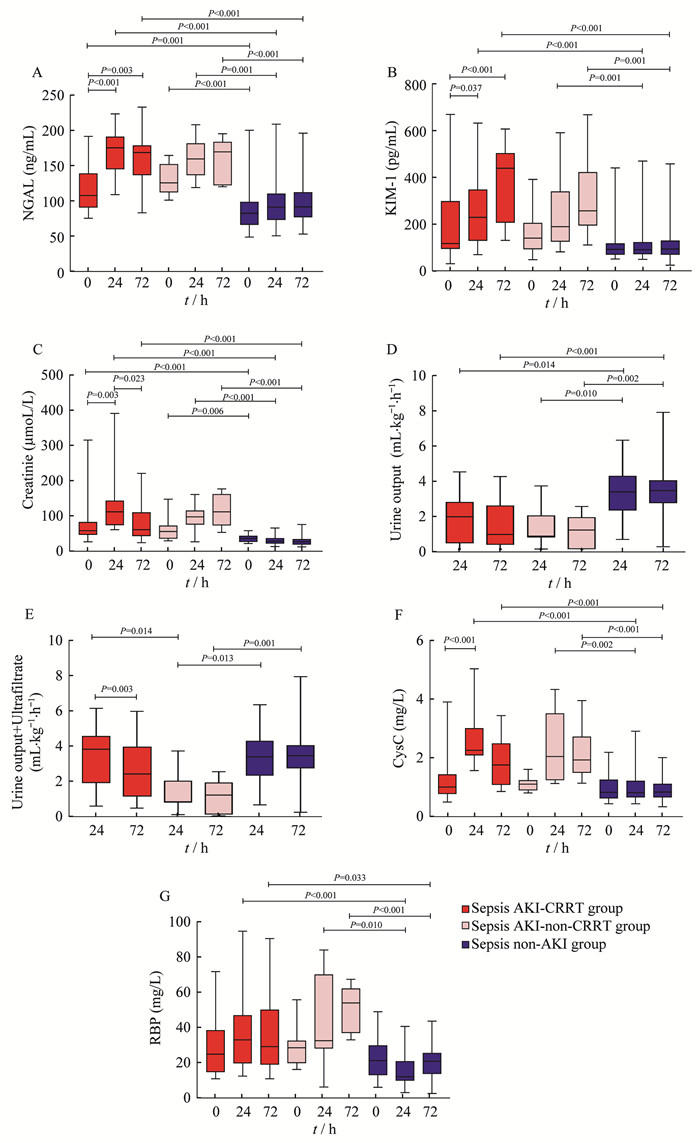
脓毒症AKI-CRRT组、脓毒症AKI-非CRRT组和脓毒症非AKI组各指标检测结果比较 0 h及之后各观察时点,NGAL、肌酐在脓毒症AKI-CRRT组和脓毒症AKI非CRRT组的检测水平均高于脓毒症非AKI组(P均 < 0.05)。KIM-1、CysC、RBP在24 h和72 h时,脓毒症AKI-CRRT组及非CRRT组患儿均高于脓毒症非AKI组(P均 < 0.05)。脓毒症AKI患者无论是否进行CRRT治疗,尿量均低于脓毒症非AKI组,CRRT治疗组24 h时点的尿量+超滤量高于非CRRT组(P均 < 0.05)。进行CRRT治疗的脓毒症AKI患儿,与0 h时点相比,肌酐在24 h显著升高,72 h较24 h明显下降(P均 < 0.05),NGAL、KIM-1、CysC在24 h显著升高后保持平稳(P均 < 0.05),尿量、RBP在各时点均无显著变化(图 1A~G)。
|
| AKI:Acute kidney injury; CRRT:Continuous renal replacement therapy. 图 1 脓毒症AKI-CRRT组和非CRRT组及脓毒症非AKI组各检测指标的比较 Fig 1 Comparison of various biomarkers among sepsis AKI-CRRT group, sepsis AKI-non-CRRT group and sepsis non-AKI group |
经CRRT治疗的脓毒症-AKI患儿各指标诊断价值比较 NGAL在0 h时的AUC面积最大(0.907),敏感度最高(92%),特异性最强(78.6%)。24 h时NGAL、KIM-1、肌酐和CysC均显示良好的诊断效能,NGAL仍显示了最高的敏感性(96%)和特异性(98.6%)。72 h时NGAL和KIM-1的诊断效能优于其他指标,两指标的AUC面积均 > 0.9,敏感度 > 90%,特异性87.1%,肌酐在72 h的的诊断敏感度降低至88%,特异性降至77.1%(P < 0.05)。RBP各时点的AUC面积均 < 0.8,敏感度≤60%(表 3)。
| Biomarker | AUC | 95%CI | Cut-off value | P | Sensitivity (%) | Specificity (%) |
| 0 h | ||||||
| NGAL | 0.907 | 0.848-0.966 | 89.28 ng/mL | < 0.001 | 92 | 78.6 |
| KIM-1 | 0.783 | 0.680-0.887 | 91.04 pg/mL | < 0.001 | 80 | 71.4 |
| Creatinine | 0.816 | 0.716-0.917 | 47.50 μmol/L | < 0.001 | 72 | 78.6 |
| Urine output | - | - | - | - | - | |
| CysC | 0.685 | 0.560-0.810 | 0.94 mg/L | 0.006 | 68 | 67.1 |
| RBP | 0.560 | 0.417-0.702 | 29.70 mg/L | 0.377 | 44 | 77.1 |
| 24 h | ||||||
| NGAL | 0.985 | 0.960-1.000 | 128.18 ng/mL | < 0.001 | 96 | 98.6 |
| KIM-1 | 0.894 | 0.830-0.959 | 102.19 pg/mL | < 0.001 | 92 | 77.1 |
| Creatinine | 0.970 | 0.923-1.000 | 64.00 μmol/L | < 0.001 | 92 | 95.7 |
| Urine output | 0.766 | 0.642-0.889 | 2.06 mL·kg-1·h-1 | < 0.001 | 64 | 85.4 |
| CysC | 0.977 | 0.950-1.000 | 1.55 mg/L | < 0.001 | 92 | 97.1 |
| RBP | 0.754 | 0.631-0.877 | 32.15 mg/L | 0.001 | 56 | 91.4 |
| 72 h | ||||||
| NGAL | 0.933 | 0.881-0.984 | 117.40 ng/mL | < 0.001 | 92 | 87.1 |
| KIM-1 | 0.957 | 0.920-0.993 | 128.14 pg/mL | < 0.001 | 96 | 87.1 |
| Creatinine | 0.887 | 0.812-0.963 | 42.00 μmol/L | < 0.001 | 88 | 77.1 |
| Urine output | 0.844 | 0.742-0.947 | 2.58 mL·kg-1·h-1 | < 0.001 | 84 | 80.5 |
| CysC | 0.919 | 0.860-0.977 | 1.33 mg/L | < 0.001 | 72 | 95.7 |
| RBP | 0.739 | 0.603-0.876 | 34.65 mg/L | 0.001 | 60 | 94.3 |
未经CRRT治疗的脓毒症AKI患儿各指标的诊断价值比较 比较脓毒症AKI-非CRRT治疗组ROC曲线,NGAL在0 h时AUC面积最大(0.951),敏感度最高(100%),特异性87.1%,肌酐在该时点的AUC面积较小(0.751),敏感度最低(42.9%)。24 h时NGAL、KIM-1、肌酐和CysC均显示良好的诊断效能,NGAL仍显示了最高的敏感度(100%)和特异性(98.6%)。72 h时除尿量外,其余各检测指标的AUC均 > 0.9(表 4)。
| Biomarker | AUC | 95%CI | Cut-off value | P | Sensitivity (%) | Specificity (%) |
| 0 h | ||||||
| NGAL | 0.951 | 0.902-1.000 | 100.88 ng/mL | < 0.001 | 100 | 87.1 |
| KIM-1 | 0.753 | 0.584-0.922 | 98.15 pg/mL | 0.028 | 71.4 | 78.6 |
| Creatinine | 0.751 | 0.559-0.943 | 70.50 μmol/L | 0.029 | 42.9 | 100 |
| Urine output | - | - | - | - | - | |
| CysC | 0.758 | 0.627-0.810 | 0.80 mg/L | 0.025 | 100 | 50 |
| RBP | 0.600 | 0.383-0.817 | 28.35 mg/L | 0.385 | 57.1 | 70 |
| 24 h | ||||||
| NGAL | 0.990 | 0.969-1.000 | 134.75 ng/mL | < 0.001 | 100 | 98.6 |
| KIM-1 | 0.880 | 0.782-0.978 | 112.84 pg/mL | 0.001 | 85.7 | 81.4 |
| Creatinine | 0.913 | 0.758-1.000 | 66.00 μmol/L | < 0.001 | 85.7 | 98.6 |
| Urine output | 0.778 | 0.608-0.949 | 2.06 mL·kg-1·h-1 | 0.017 | 85.7 | 72.9 |
| CysC | 0.946 | 0.883-1.000 | 1.13 mg/L | < 0.001 | 100 | 80 |
| RBP | 0.804 | 0.569-1.000 | 28.25 mg/L | 0.008 | 85.7 | 81.4 |
| 72 h | ||||||
| NGAL | 0.957 | 0.910-1.000 | 117.40 ng/mL | < 0.001 | 100 | 87.1 |
| KIM-1 | 0.939 | 0.871-1.000 | 108.42 pg/mL | < 0.001 | 100 | 77.1 |
| Creatinine | 0.976 | 0.934-1.000 | 52.50 μmol/L | < 0.001 | 100 | 85.7 |
| Urine output | 0.805 | 0.688-0.922 | 2.58 mL·kg-1·h-1 | 0.009 | 100 | 62.7 |
| CysC | 0.970 | 0.929-1.000 | 1.13 mg/L | < 0.001 | 100 | 85.7 |
| RBP | 0.977 | 0.943-1.000 | 33.05 mg/L | < 0.001 | 100 | 90 |
目前,有文献报道脓毒症合并AKI的机制是中性粒细胞、单核细胞以及血管内皮细胞发生复杂交错的免疫反应,肾小管在炎症细胞的浸润下,细胞发生自噬、凋亡以及坏死,最终造成肾小管受损而引发AKI[11-13]。在众多新的生物标志物中,研究最多且最有临床应用前景的是NGAL和KIM-1。NGAL主要来源于中性粒细胞,少量表达于肾、脾、肝,与明胶酶B相关,相对分子质量为25 000[14]。KIM-1是来源于肾脏近曲小管上皮细胞的I型膜糖蛋白,相对分子质量39 000[15]。研究显示NGAL、KIM-1可对先天性心脏病患儿体外循环(cardiopulmonary bypass,CPB)术后诱发的AKI进行预测和诊断[16-17]。近年来的研究认为这2个生物大分子标志物对脓毒症、接受冠状动脉造影的急性冠脉综合征或心力衰竭患者、泌尿系统疾病所致AKI有较好的早期诊断价值[18-21]。
在0 h、24 h、72 h的动态监测中发现:脓毒症AKI组的NGAL、KIM-1水平均明显高于非AKI患儿和正常对照组。当机体发生脓毒症时,在细菌内毒素的刺激下释放出大量内源性的炎症介质,不仅对肾小管造成不同程度的损伤,从而导致AKI的发生,还会促进肾小管上皮细胞产生NGAL,因此脓毒症引发AKI时NGAL明显升高[22-24]。KIM-1来源于肾小管上皮细胞,在上皮细胞损伤时表达增强,且持续至上皮细胞修复[25]。研究认为AKI引发了ERK1/2、STAT3磷酸化,STAT3与KIM-1启动子结合,增加其mRNA和蛋白质水平,KIM-1细胞外结构域的脱落导致血液或尿液中KIM-1水平大大增加[26]。国外有研究显示,检测尿NGAL易受尿液中白细胞的干扰影响,因此本研究采用血液标本替代尿液标本。
本研究中有18例脓毒症AKI组患儿在诊断AKI后进行了CRRT。0 h时脓毒症AKI-CRRT组和脓毒症AKI-非CRRT组的NGAL和肌酐水平都明显高于脓毒症非AKI组;两组脓毒症AKI患儿中,NGAL的AUC面积均最大(分别为0.907和0.951),敏感度最高(分别为92%和100%),特异性强(分别为78.6%和87.1%),对脓毒症AKI的诊断效能优于其他指标。国内研究报道,成人脓毒症患者NGAL预测AKI较肌酐可至少提前6 h[27-29],在儿童中NGAL预测AKI的时间可提早24 h[30-31]。张辉等[32]对92例儿童AKI标志物的研究显示,虽在达到AKI诊断标准时肌酐的诊断特异性最好,但血肌酐的变化往往滞后于肾功能的改变,当肌酐升高程度达到诊断标准时,患儿病情已较为严重,因此肌酐的变化对AKI的早期诊断缺乏高敏感性。由于0 h时无法计算尿量,借助尿量诊断AKI需要一定的观察时间,所以依靠尿量对AKI的诊断存在滞后。0 h时CysC、RBP水平在脓毒症AKI-CRRT组、脓毒症AKI-非CRRT组和脓毒症非AKI组3组间比较均没有显著差异,提示CysC与RBP无法在早期有效区分脓毒症是否合并AKI。NGAL在疾病早期显著增高,因此临床检测NGAL可以更早地帮助预警AKI的发生,从而达到尽早干预的目的。
在行CRRT治疗的AKI患儿各时点的动态监测中观察到:72 h与24 h肌酐水平相比呈现下降趋势,并且72 h较24 h肌酐的AUC面积减小、敏感度和特异性均降低;而NGAL、KIM-1分别在24 h显著升高后,至72 h仍维持在较高水平,且NGAL在3个时点和KIM-1在后2个时点均维持良好的诊断效能。而脓毒症AKI组中未行CRRT治疗的患儿,各指标在72 h与24 h相比,AUC面积、敏感度和特异性均没有明显的变化。分析认为:目前临床应用的CRRT滤器均采用高通量滤器,其对溶质清除截点(cut off)为20 000~250 000,这5个生物标志物的相对分子质量(Mr)从小到大依次为:肌酐(113) < CysC(13 000) < RBP(21 000) < NGAL(25 000) < KIM-1(39 000)[33]。可见在CRRT治疗过程中,“金标准”肌酐易被滤过,从而不能反映肾功能真实情况。而NGAL和KIM-1的相对分子质量均 > 20 000,理论上在CRRT治疗进程中不易被清除,从而继续维持相对稳定的高水平表达。CysC和RBP的相对分子质量与清除截点接近,也可能受到一定的影响。尿量在脓毒症AKI-CRRT治疗组和非CRRT治疗组比较结果没有显著差异,但当将尿量加上CRRT治疗过程中滤出体内的超滤量,24 h时脓毒症AKI-CRRT组则高于非CRRT组。可见,CRRT治疗期间由于应用了超滤模式替代肾脏排尿功能,患儿实际产生的尿量与其真实的肾功能不相符,所以无法在行CRRT过程中应用尿量反映肾功能真实情况。如需通过尿量反映AKI病情的进展,则要等待治疗间隙观察后再作评估,显然尿量无法与治疗保持同步的测量。与此同时,脓毒症采用集束化治疗,临床应用药物(如利尿剂)、透析等方式均有可能干扰诊断的效率。从脓毒症AKI-CRRT组ROC曲线比较结果来看,NGAL在3个时点、KIM-1在后2个时点均保持较高敏感性及特异性,验证了大分子标志物NAGL和KIM-1能够更有效地反映CRRT治疗后肾功能的真实情况[34-36]。
本研究的不足之处是儿童脓毒症病例数较少,仅为小样本量研究,得到的是初步结果,后续拟增大样本量进一步研究NGAL和KIM-1的诊断价值。
综上所述,重症患儿且同时诊断脓毒症和AKI时病情复杂并发展迅速,病程中多个生物标志物的动态监测显示NGAL灵敏度高,对AKI的发生可能起到早期提示作用,而在血液净化的治疗过程中NGAL和KIM-1受干扰因素较少,可对这些患儿肾功能真实水平的评估提供更多的诊断指标。
作者贡献声明 徐佳音 论文构思,执行实验,数据采集,统计分析,撰写和修订论文。朱海燕 文献调研和整理,执行实验,数据采集。徐锦 研究指导,论文修订。
利益冲突声明 所有作者均声明不存在利益冲突。
| [1] |
SINGER M, DEUTSCHMAN CS, SEYMOUR CW, et al. The third international consensus definitions for sepsis and septic shock (Sepsis-3)[J]. JAMA, 2016, 315(8): 801-810.
[DOI]
|
| [2] |
CHANG JW, JENG MJ, YANG LY, et al. The epidemiology and prognostic factors of mortality in critically ill children with acute kidney injury in Taiwan[J]. Kidney Int, 2015, 87(3): 632-639.
[DOI]
|
| [3] |
SCHLAPBACH LJ, STRANEY L, ALEXANDER J, et al. Mortality related to invasive infections, sepsis, and septic shock in critically ill children in Australia and New Zealand, 2002-13:a multicentre retrospective cohort study[J]. The Lancet Infect Dis, 2015, 15(1): 46-54.
[DOI]
|
| [4] |
KHWAJA A. KDIGO Clinical Practice Guidelines For Acute Kidney Injury[J]. Nephron Clin Pract, 2012, 120(4): 179-184.
[URI]
|
| [5] |
耿海云, 陈朝英, 涂娟. 儿童住院患者急性肾损伤的发病情况[J]. 中华肾脏病志, 2017, 33(8): 595-600. [URI]
|
| [6] |
中华医学会儿科学分会急救学组, 中华医学会急诊医学分会儿科学组, 中国医师协会儿童重症医师分会. 儿童脓毒性休克(感染性休克)诊治专家共识(2015版)[J]. 中华实用儿科临床杂志, 2015, 30(22): 1687-1691. [DOI]
|
| [7] |
VINSONNEAU C, ALLAIN-LAUNAY E, BLAYAU C, et al. Renal replacement therapy in adult and pediatric intensive care:recommendations by an expert panel from the French Intensive Care Society (SRLF) with the French Society of Anesthesia Intensive Care (SFAR) French Group for Pediatric Intensive Care Emergencies (GFRUP) the French Dialysis Society (SFD)[J]. Ann Intensive Care, 2015, 5(1): 58.
[DOI]
|
| [8] |
RHODES A, EVANS LE, ALHAZZANI W, et al. Surviving sepsis campaign:international guidelines for management of sepsis and septic shock:2016[J]. Intensive Care Med, 2017, 43(3): 304-377.
|
| [9] |
NI X, SONG WQ, PENG XX, et al. Pediatric reference intervals in China(PRINCE):design and rationale for a large, multicenter collaborative cross-sectional study[J]. Sci Bull, 2018, 63(24): 34-42.
|
| [10] |
WS-T/S402-2012.临床实验室检验项目参考区间的制定[S].北京: 中华人民共和国卫生部, 2012.
|
| [11] |
ISHIKAWA K, MAY CN, GOBE G, et al. Pathophysiology of septic acute kidney injury:a different view of tubular injury[J]. Contrib Nephrol, 2010, 165: 18-27.
[DOI]
|
| [12] |
PROWLE JR, BELLOMO R. Sepsis-associated acute kidney injury:macrohemodynamic and microhemodynamic alterations in the renal circulation[J]. Semin Nephrol, 2015, 35(1): 64-74.
[DOI]
|
| [13] |
FANI F, REGOLISTI G, DELSANTE M, et al. Recent advances in the pathogenetic mechanisms of sepsis-associated acute kidney injury[J]. J Nephrol, 2018, 31(3): 351-359.
[DOI]
|
| [14] |
KJELDSEN L, JOHNSEN AH, SENGELØV H, et al. Isolation and primary structure of NGAL, a novel protein associated with human neutrophil gelatinase[J]. J Biol Chem, 1993, 268(14): 10425-10432.
[DOI]
|
| [15] |
ICHIMURA T. Kidney injury molecule-1(KIM-1), a putative epithelial cell adhesion molecule containing a novel immunoglobulin domain, is up-regulated in renal cells after injury[J]. J Biol Chem, 1998, 273(7): 4135-4142.
[DOI]
|
| [16] |
MISHRA J, DENT C, TARABISHI R, et al. Neutrophil gelatinase-associated lipocalin (NGAL) as a biomarker for acute renal injury after cardiac surgery[J]. Lancet, 2005, 365(9466): 1231-1238.
[DOI]
|
| [17] |
LIANG XL, LIU SX, CHEN YH, et al. Combination of urinary kidney injury molecule-1 and interleukin-18 as early biomarker for the diagnosis and progressive assessment of acute kidney injury following cardiopulmonary bypass surgery:a prospective nested case-control study[J]. Biomarkers, 2010, 15(4): 332-339.
[DOI]
|
| [18] |
TORREGROSA I, MONTOLIU C, URIOS A, et al. Urinary KIM-1, NGAL and L-FABP for the diagnosis of AKI in patients with acute coronary syndrome or heart failure undergoing coronary angiography[J]. Heart Vessels, 2015, 30(6): 703-711.
[DOI]
|
| [19] |
许光银, 乔彩霞, 王志玉. 多项生物学标志物联合检测在重症患者合并急性肾损伤早期诊断中的价值[J]. 中华肾脏病杂志, 2014, 30(3): 166-171. [DOI]
|
| [20] |
侯玲, 杜悦, 郭金杰. 血清和尿中NGAL、KIM-1水平在儿童泌尿系统疾病致急性肾损伤诊断中的作用[J]. 中国医科大学学报, 2013, 42(7): 619-622. [DOI]
|
| [21] |
CHAO-WEI L, HAO-WEI K, HONG-SHIUE C, et al. A combination of SOFA score and biomarkers gives a better prediction of septic AKI and in-hospital mortality in critically ill surgical patients:a pilot study[J]. World J Emerg Surg, 2018, 13(1): 41.
[DOI]
|
| [22] |
AIRD WC. The role of the endothelium in severe sepsis and multiple organ dysfunction syndrome[J]. Blood, 2003, 101(10): 3765-3777.
[DOI]
|
| [23] |
MISHRA J. Identification of Neutrophil gelatinase-associated lipocalin as a novel early urinary biomarker for ischemic renal injury[J]. J Am Soc Nephrol, 2003, 14(10): 2534-2543.
[DOI]
|
| [24] |
BONNEMAISON ML, MARKS ES, BOESEN EI. Interleukin-1β as a driver of renal NGAL production[J]. Cytokine, 2017, 91: 38-43.
[DOI]
|
| [25] |
SABBISETTI VS, WAIKAR SS, ANTOINE DJ, et al. Blood kidney injury molecule-1 is a biomarker of acute and chronic kidney injury and predicts progression to ESRD in type Ⅰ diabetes[J]. J Am Soc Nephrol, 2014, 25(10): 2177-2186.
[DOI]
|
| [26] |
COLLIER JB, SCHNELLMANN RG. Extracellular signal-regulated kinase 1/2 regulates mouse kidney injury molecule-1 expression physiologically and following ischemic and septic renal injury[J]. J Pharmacol Exp Ther, 2017, 363(3): 419-427.
[DOI]
|
| [27] |
CULLEN MR, MURRAY PT, FITZGIBBON MC. Establishment of a reference interval for urinary neutrophil gelatinase-associated lipocalin[J]. Ann Clin Biochem, 2012, 49(2): 190-193.
[DOI]
|
| [28] |
朱丽丽, 师东武. 中性粒细胞明胶酶相关脂质运载蛋白及白细胞介素-18在脓毒症所致急性肾损伤中的早期诊断价值[J]. 中华危重病急救医学, 2016, 28(8): 718-722. [DOI]
|
| [29] |
李萍珠, 徐炜新. 脓毒血症并发急性肾损伤早期诊断标志物的研究[J]. 中华检验医学杂志, 2010, 33(6): 492-496. [DOI]
|
| [30] |
郑静, 何海兰, 张国英. 人中性粒细胞明胶酶相关性脂质运载蛋白对ICU儿童脓毒症致急性肾损伤的预测诊断价值[J]. 第三军医大学学报, 2017, 39(2): 196-200. [CNKI]
|
| [31] |
VAIDYA VS, OZER JS, DIETERLE F, et al. Kidney injury molecule-1 outperforms traditional biomarkers of kidney injury in preclinical biomarker qualification studies[J]. Nature Biotechnol, 2010, 28(5): 478-485.
[DOI]
|
| [32] |
张辉, 易著文, 肖政辉. 脓毒症急性肾损伤相关指标间的关系[J]. 临床儿科杂志, 2015, 33(12): 1021-1026. [DOI]
|
| [33] |
RONCO C. Continuous renal replacement therapy:forty-year anniversary[J]. Int J Artif Organs, 2017, 40(6): 257-264.
[DOI]
|
| [34] |
RONCO C, LEGRAND M, GOLDSTEIN SL, et al. Neutrophil gelatinase-associated lipocalin:ready for routine clinical use?An international perspective[J]. Blood Purif, 2014, 37(4): 271-285.
[DOI]
|
| [35] |
CHANG W, ZHU S, PAN C, et al. Predictive utilities of neutrophil gelatinase-associated lipocalin (NGAL) in severe sepsis[J]. Clin Chim Acta, 2018, 481: 200-206.
[DOI]
|
| [36] |
SHAO YM, FAN YQ, XIE YL, et al. Effect of continuous renal replacement therapy on kidney injury molecule-1 and neutrophil gelatinase-associated lipocalin in patients with septic acute kidney injury[J]. Exp Ther Med, 2017, 13(6): 3594-3602.
[DOI]
|
 2021, Vol. 48
2021, Vol. 48


